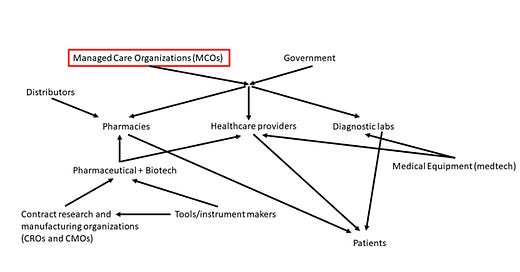
Deep Dive into Managed Care Organizations (MCOs), part 2
Why $UNH is an attractive opportunity here
The largest MCOs by market cap are UnitedHealth, Anthem, and CVS. Each of these have slightly different strategies they pursue within their insurance and non-insurance parts of their business. Their business mix is detailed below:
Non-insurance part of MCOs breakdown
So what is the non-insurance part of these companies? The answer is that it differs by company:
UnitedHealth has the most diverse umbrella of non-insurance businesses under their Optum brand that accounts for 45% of total EBIT. Under here, there is a pharmacy benefits manager (PBM) called OptumRx, a healthcare provider business called OptumCare, and a data and analytics business called OptumInsights. By the way, a PBM is an intermediary between pharma and biotech companies and pharmacies that negotiate better rates for pharmaceutical drugs on behalf of pharmacies. CVS’ non-insurance business includes a PBM and ~10k CVS-branded retail pharmacies. Anthem has the smallest non-insurance business of the three that mainly includes a PBM business. What’s common between all these three MCOs is that they are pursuing a vertical integration model but some like UnitedHealth are ahead of others like Anthem and some like CVS are pursuing a different flavour of vertical integration vis-à-vis retail pharmacies vs others like UnitedHealth vis-à-vis healthcare providers (ie., OptumCare) and software (ie., OptumInsights).
You may ask the question of why MCOs are so keen on vertical integration? This is an especially important question given the negative connotation with vertical integration from companies in other industries like Intel. Briefly, Intel pursued a vertical integration model in that both design and manufacturing was done in-house, and they are now losing market share to AMD, which focused on design and outsourced manufacturing. The chief problem here was that Intel did not benefit from economies of scale in manufacturing to the same extent as AMD as the outsourcing/specialization model allows for more scale over time.
Back to the matter at hand, why does vertical integration make sense for MCOs? A few reasons why: 1) the insurance part of the business is regulated and for the most part, margins are capped in this business but the same is not the case for the non-insurance part of the business (ie., allows for higher margins of the consolidated business); 2) some of these non-insurance businesses like PBMs are highly complementary to the insurance business and it helps in sales pitches to potential clients to have ancillary services like this (ie., higher win rates à higher revenues); 3) MCOs are able to steer their members to specific healthcare providers or pharmacies in order to increase utilization rate and as such, they can increase scale at these acquired targets provided they have enough local traffic that they can steer there (ie., higher revenues for acquired businesses, aka revenue synergies).
But I don’t want to carry this vertical integration argument too far as the businesses still have to make sense on a stand-alone basis. For instance, I would be concerned if UnitedHealth was buying hospitals that are typically higher cost than urgent care centers that UnitedHealth is buying. By buying lower cost healthcare providers and steering additional traffic to these centers, UnitedHealth is offering a win-win proposition to all stakeholders by simultaneously lowering the cost of healthcare, improving the quality of healthcare (lower incidence of infectious diseases in urgent care centers vs hospitals), and improving economics of acquired targets. Another example of this is to look at CVS’ retail pharmacy business, which is losing market share to other brick-and-mortar retailer and to e-commerce that can offer front-of-item consumer goods like toilet paper and food snacks for as much as 40% cheaper. In my view, this is an example of vertical integration wherein the stand-alone business does not pass the sniff-test, but this is also reflected in the valuation (CVS trades at ~1/2 the fwd P/E multiple as UnitedHealth).
One less appreciated moat for these companies is the rich data that they have access to in the process of coordinating healthcare for their members. UnitedHealth, for instance, is estimated to have access to ~1/2 of all claims information in the US from both what they see from their own members and what they see via Optum services from non-members (for eg., OptumInsights works with several hospitals to process revenues and is agnostic to patients’ payers).
Economic evidence of owning non-regulated, high-quality businesses is a higher margin and it is no surprise that UnitedHealth has the highest consolidated EBIT margin of all MCOs at 9% vs 7% for Anthem and 5% for CVS. It is also no surprise that UnitedHealth has seen an EBIT margin expansion of ~200bps over the past 5yrs as the non-insurance part of the business has outgrown the insurance part of the business.
Insurance part of MCOs breakdown
The insurance parts of these MCOs also have their nuances across companies. One of these nuances is the member mix with UnitedHealth having a higher mix of Medicare relative to Medicaid members, for instance, than Anthem, which has a higher mix of Medicaid relative to Medicare members. The nuances do not matter that much except to say that commercial is largely a saturated customer base with little volume growth opportunity but still price growth of 2-6% from healthcare inflation. In contrast, both Medicare and Medicaid are higher growth opportunities due to incremental outsourcing of government healthcare spend to MCOs (see part 1 for more detail), and there is additional price growth from healthcare inflation.
Customer acquisition is a little different across the MCOs. Anthem is unique in that it is the largest licensee of Blue Cross Blue Shield, which is a ~90yr old brand associated with healthcare insurance. This allows Anthem to tap into the much larger member base of Blue Cross Blue Shield (covering ~40% of insured members in the US vs ~20% for #2 player UnitedHealth) and to access their economies of scale across a wider network. But this competitive advantage is mainly for commercial members, which are a saturated sub-population as described above.
Note that in the table above, UnitedHealth has the highest exposure to Medicare + Medicaid members (39% of total) and as a result, is expected to have the highest growth rate of the three MCOs within the insurance part of the business.
How does valuation compare?
Valuation is very different between the three MCOs reflecting many of the differences in the business mix and quality as discussed above. A couple of valuation metrics are shown below.
*using 2019 as MCOs experienced a windfall in 2020 due to the pandemic that resulted in fewer elective surgeries and lower claims payouts for the MCOs. As this is unsustainable, used FCF from a more normal year, ie., 2019.
What is more interesting is not how the valuation differs between MCOs, but instead how the valuation differs between MCOs and the broader market. Even the most expensive MCO, UnitedHealth, is similar in valuation on a forward P/E basis as the S&P 500 index while it is arguably a compounder having grown FCF at 14% over the past 12 years. With ample room for further growth both on government portion of insurance and on parts of the non-insurance portion of the businesses and a relatively resilient business, MCOs are a good portfolio option to own. I like UnitedHealth for the reasons discussed above, and think that the valuation is still very attractive for the growth you get relative to other options both within and outside of the healthcare value chain.